8.3 Diagnostic Imaging: Radiology
The Origins of X-Rays
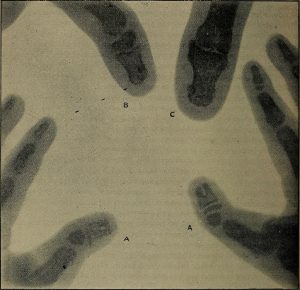
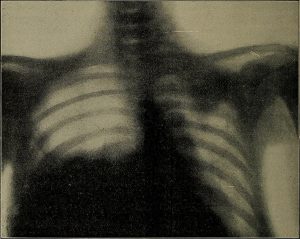
In 1895, German physicist Wilhelm Röntgen was experimenting with electrical current when he discovered that invisible “rays” could pass through his flesh and leave an outline of his bones on a screen coated with a metal compound (Betts et al., 2013). He then made the first record of the internal parts of a living human with an image of his wife’s hand. This record eventually became known as an “X-ray.” Once this discovery was made, advancements came quickly, and by 1900, X-rays had become widely used. They could detect a variety of injuries and diseases, which led to great advancements in patient care and outcomes (Betts et al., 2013). Fig. 8.12 and Fig. 8.13 show some of the early X-rays taken by Röntgen.
Modern Use of X-Rays
The use of X-rays is commonplace in health care today, and most people have had at least one X-ray (Betts et al., 2013). Even though they are very common, most of us do not know how X-rays work. X-rays are emitted from a specialized machine that directs the rays through a particular part of the body and toward a specially treated metallic plate. The beam of radiation from the X-ray machine results in darkening of the X-ray plate (Betts et al., 2013). Different tissues show up as different shades; X-rays are only slightly impeded by soft tissues, which show up as varying shades pf grey, whereas hard tissues, such as bone, block the rays and appear white. Metal and contrast dyes also appear white. Structures containing air will look black. As a result, X-rays are best used to visualize hard body structures such as teeth and bones (Betts et al., 2013).
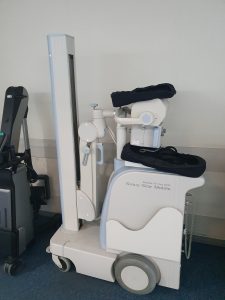
X-rays can depict a two-dimensional image of any body region but only from a single angle (Betts et al., 2013). If a more detailed or three-dimensional image is needed, then another form of test would be indicated and these will be discussed later in the chapter. The two figures below show examples of both portable (Fig. 8.14) and stationary (Fig. 8.15) X-ray machines.

Specific Types of X-Rays
A selection of different types of X-rays and specialty tests are discussed below. They are, of course, not all the possible tests, but they will give you a foundation of knowledge of the common types of X-rays that are key aspects of patient care in a medical setting.
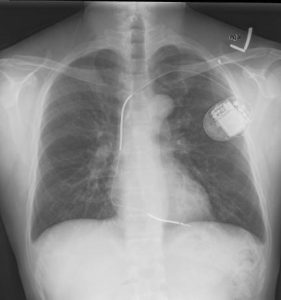
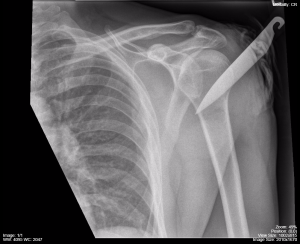
Chest X-ray (CXR): This is a very common form of X-ray and can be used in cases of trauma, pain, or illness. A CXR can help diagnose infections such as pneumonia or an accumulation of fluid such as pleural effusion. It can be very helpful in treating various forms of trauma; for example, in Fig. 8.16, the patient was stabbed with a knife. Fig. 8.17 shows a patient who has an implanted defibrillator but no other anomalies.
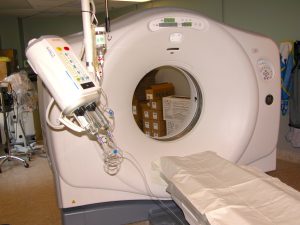
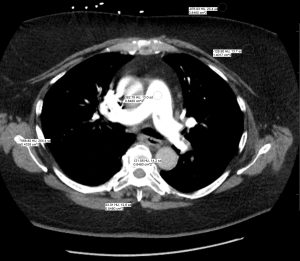
Computed tomography (CT): A CT is a type of X-ray that shows images in cross-section, which provides much more detail and helps to assess a patient. Although not always used, contrast material (dye) can be injected into the bloodstream to highlight structures; for example, for a liver CT. During a CT, the patient lies on a horizontal table, and the X-ray tube, which is in a ring assembly, spins around the patient, as can be seen in Fig. 8.18. Fig. 8.19 shows an example of a CT scan.
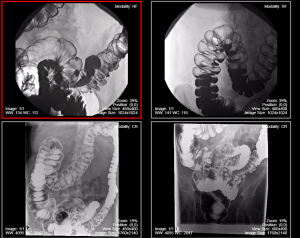
Barium (Ba) tests: To better visualize internal organs, some X-rays use a contrast medium called barium that is swallowed or given to the patient in the form of an enema. When tissues are very similar in appearance to the structures around them, the barium helps differentiate them. Malignant tissues, for example, often display differently when contrast is used compared to normal tissues. Fig. 8.20 is an example of an X-ray with barium contrast.
Key Concept
Barium is just one type of contrast medium. There are a number of different forms of imaging contrast (gas, liquid, suspension) that can be delivered by mouth, per rectum, or via intravenous or intraarterial routes. Each delivery mode has unique uses and applications in diagnostic imaging.
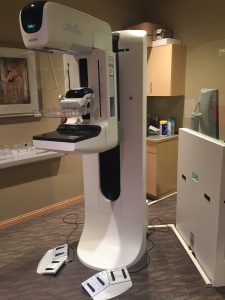
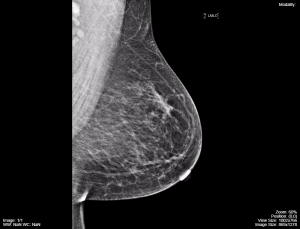
Mammography: This test creates images by passing X-rays through breast tissue. Mammography is predominantly used to image female breast tissue, as can be seen in Fig. 8.22, but it is also capable of imaging male breast tissue to assess a palpable nodule or mass. This test is often ordered as part of a regular health screen, as well as in cases where anomalies, such as cysts or tumours, may be present. Fig. 8.21 shows the machine used to take mammograms, and Fig. 8.22 is a mammogram image.
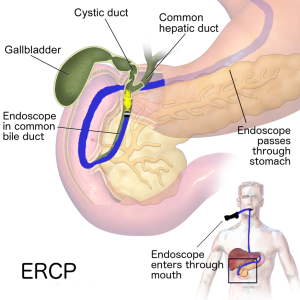
Endoscopic retrograde cholangiopancreatography (ERCP): An ERCP is a complex procedure that combines an upper gastrointestinal endoscopy and an X-ray (NIDDK, 2016). It is used to diagnose and treat issues in the bile and pancreatic ducts. Fig. 8.23 shows the procedure being performed, and Fig. 8.24 is an example of how a scan would look when completed.

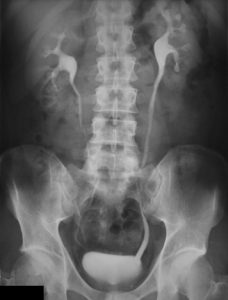
Urography: This test is used to evaluate the kidneys, ureters, and bladder. It can be used to diagnose anomalies such as cancer and assist with assessing patients experiencing abnormal urinary symptoms such as hematuria. Urography is very similar to a kidney, ureters, bladder (KUB) X-ray, which also provides imagining of the organs and structures of the urinary and gastrointestinal systems. Fig. 8.25 and Fig. 8.26 show examples of urograms.

Fluoroscopy: This test uses live X-rays to visualize anatomic structures. It is best used to depict active physical movements, including intestinal peristalsis or swallowing; for example, an esophogram and upper gastrointestinal series. Fluoroscopy is shown in the video below, which shows a patient swallowing barium sulphate and gas-forming granules. The barium can be seen moving down the esophagus and digestive tract while the gas rises to the highest point of the intestinal tract based on the patient’s position. The barium and gas help outline the inner lining of the esophagus and the intestines.
Video credit: Burbridge, B. (n.d.). Fluoroscopy of the pharynx and upper esophagus [Video]. In E. Mah & B. Burbridge, Undergraduate Diagnostic Imaging Fundamentals: Chapter 3: Fluoroscopy. University of Saskatchewan. https://openpress.usask.ca/app/uploads/sites/34/2019/02/3.17-Fluoroscopy-cine-2.mp4, licensed under CC-BY-NC-SA 4.0
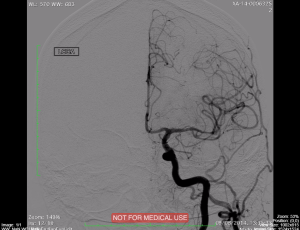
Angiography: This test uses a fluoroscopy unit with advanced features, including software applications to assist with complex arterial and body interventional procedures beyond the capabilities of a normal fluoroscopy unit. Fig. 8.27 shows an angiography machine, and Fig. 8.28 provides an example of a cardiac angiogram.

Key Concept
Cardiac catheterization (often called cardiac cath or coronary angiogram) involves

placing a very small, flexible catheter into a blood vessel in the groin, arm, or neck (Johns Hopkins, 2022). The catheter is then passed through the blood vessel into the aorta and into the heart. Once the catheter is in position, several tests may be done, including measuring the pressure within the heart chamber, recording oxygen levels, and taking blood samples (Johns Hopkins, 2022). Contrast dye can be injected to check blood flow, while X-rays are used to assist with visualization.
Exercises
Attribution
Unless otherwise indicated, material on this page has been adapted from the following resource:
Burbridge, B. (2017). Undergraduate diagnostic imaging fundamentals. University of Saskatchewan, Distance Education Unit. https://openpress.usask.ca/undergradimaging/ licensed under CC BY-NC-SA 4.0
References
Betts, J. G., Young, K. A., Wise, J. A., Johnson, E., Poe, B., Kruse, D. H., Korol, O., Johnson, J. E., Womble, M., & DeSaix, P. (2013). Anatomy and physiology. OpenStax. https://openstax.org/details/books/anatomy-and-physiology licensed under CC BY 4.0
Johns Hopkins. (2022). Cardiac catheterization. https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/cardiac-catheterization#:~:text=In%20cardiac%20catheterization%20(often%20called,several%20tests%20may%20be%20done
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). (2016). Endoscopic retrograde cholangiopancreatography (ERCP). https://www.niddk.nih.gov/health-information/diagnostic-tests/endoscopic-retrograde-cholangiopancreatography
Image Credits (images are listed in order of appearance)
The Röntgen rays in medical work (1899) (14570499897) by Internet Archive Book Images, Public domain
The Röntgen rays in medical work (1899) (14756957975) by Internet Archive Book Images, Public domain
Mobile X-Ray Unit Sirius Star Mobile by Syced, CC0 1.0
X-ray machine. Kaliningrad region, Russia by Government of the Kaliningrad region, CC BY 4.0
Left Shoulder X-Ray Knife by Dr. Brent Burbridge MD, CC BY-NC-SA 4.0
Implantable cardioverter defibrillator chest X-ray by Gregory Marcus, MD, CC BY 3.0
Helical CT Scanner 1 by Dr. Brent Burbridge MD, CC BY-NC-SA 4.0
Images of CT with HU measurements by Dr. Brent Burbridge MD, CC BY-NC-SA 4.0
Barium enema by Dr. Brent Burbridge MD, CC BY-NC-SA 4.0
Mammography x-ray machine 1 by Dr. Brent Burbridge MD, CC BY-NC-SA 4.0
Mammography image 3.14b by Dr. Brent Burbridge MD, CC BY-NC-SA 4.0
ERCP by Drus1a, CC BY-SA 4.0
ERCP Roentgen by J. Guntau, CC BY-SA 3.0
Medical X-Ray imaging EZX04 nevit by Nevit Dilmen, CC BY-SA 3.0
Ivu 1 by Glitzy queen00, Public domain
3.17 Fluoroscopy cine 2 by Dr. Brent Burbridge MD, CC BY-NC-SA 4.0
Angiography machine with C-arm 1 by Dr. Brent Burbridge MD, CC BY-NC-SA 4.0
Carotid angiography DSA e1506469676130 by Dr. Brent Burbridge MD, CC BY-NC-SA 4.0

